REVIEW
ARTICLE
PLANTAS
MEDICINAIS E FITOTERÁPICOS PARA TRATAMENTO DE FERIDAS CRÔNICAS: REVISÃO
INTEGRATIVA
MEDICINAL PLANTS AND PHYTOTHERAPICS FOR TREATMENT OF
CHRONIC WOUNDS: AN INTEGRATIVE REVIEW
PLANTAS MEDICINALES Y HIERBAS MEDICINALES PARA EL
TRATAMIENTO DE HERIDAS CRÓNICAS: REVISIÓN INTEGRATIVA
https://doi.org/10.31011/reaid-2026-v.100-n.1-art.2502
¹Ana Luísa Gonzaga Ferreira
2Esthefany
Belmiro Santos
3Luciana
Sousa Lins Barbosa
4Marta
Miriam Lopes Costa
5Danielly
Albuquerque da Costa
6Maria
do Socorro Sousa
¹Undergraduate
student in Nursing at the Federal University of Paraíba (UFPB), João Pessoa,
Paraíba, Brazil. ORCID: https://orcid.org/0009-0004-8787-6108.
²Undergraduate
student in Nursing at the Federal University of Paraíba (UFPB), João Pessoa,
Paraíba, Brazil. ORCID: https://orcid.org/0009-0009-8534-6847.
³Undergraduate
student in Nursing at the Federal University of Paraíba (UFPB), João Pessoa,
Paraíba, Brazil. ORCID: https://orcid.org/0009-0003-1407-2734.
4PhD in
Sociology from the Postgraduate Program in Sociology at the Federal University
of Paraíba, João Pessoa, Paraíba, Brazil. ORCID: https://orcid.org/0000-0002-2119-3935.
5Professor,
PhD, Center for Health Sciences (CCS), Department of Biomedical Sciences,
Federal University of Paraíba, João Pessoa, Paraíba, Brazil. ORCID: https://orcid.org/0000-0002-6736-4699.
6Professor,
PhD, Center for Health Sciences (CCS), Department of Biomedical Sciences,
Federal University of Paraíba, João Pessoa, Paraíba, Brazil. ORCID: https://orcid.org/0000-0002-2163-6265.
Corresponding
Author
Ana
Luísa Gonzaga Ferreira
Universidade
Federal da Paraíba – Campus I - Cidade Universitária, João Pessoa – PB, Brazil,
58051-900. Contact: +5583 987840096.
E-mail:
ana.ferreira2@academico.ufpb.br
Submission:
26-02-2025
Approval:
29-07-2025
ABSTRACT
Objective: To identify
medicinal plants and herbal medicines with healing effects used to promote the
treatment of chronic wounds. Method: This is an integrative review
conducted from January to November 2024. The articles selected for this study
were those published within the last 10 years (2013–2023) in three specific
languages: Portuguese, English, and Spanish. The following databases/libraries
were used: Biblioteca Virtual em Saúde (Virtual Health Library), Scientific
Electronic Library Online (SciELO), Portal de Periódicos da Capes (Capes
Journal Portal), Literatura Latino-Americana e do Caribe em Ciências da Saúde
(LILACS), and National Library of Medicine (PubMed). The search descriptors
included: “Medicamentos fitoterápicos” (Herbal drugs), “Feridas e lesões”
(Wounds and injuries), “Plantas medicinais” (Medicinal plants),
“Phytotherapeutic drugs”, “Wounds and injuries”, “Medicinal Plants”,
“Medicamentos fitoterapéuticos”, “Heridas y lesiones”, and “Plantas
medicinales”. Results: The search yielded 325 articles on the topic, 39
of which were available in full. After excluding those unrelated to the theme,
eight studies comprised the final sample. Focusing on the healing mechanism and
their role in the regeneration process, the review highlighted the positive impacts
of medicinal plants and/or herbal medicines in treating diverse wounds, acute
or chronic, in individuals of different ages. However, it also underscored the
scarcity of studies in this area. Conclusion: Medicinal plants with
healing properties can be used in various forms and for different purposes
depending on their compounds. The analysis of the studies demonstrates their
efficacy in treating chronic wounds.
Keywords:
Wounds;
Healing; Medicinal Plants.
RESUMEN
Objetivo: Identificar plantas medicinales
y fitoterapéuticos con efectos cicatrizantes para el tratamiento de heridas
crónicas. Método: Esta revisión integrativa se realizó de enero a noviembre de
2024, utilizando artículos publicados en los últimos 10 años (2013-2023), en
tres idiomas específicos: portugués, inglés y español, de las siguientes bases
de datos/bibliotecas: Biblioteca Virtual en Salud, Biblioteca Científica
Electrónica en Línea, Portal de Revistas de Capes, Literatura Latinoamericana y
del Caribe en Ciencias de la Salud y Biblioteca Nacional de Medicina,
utilizando los descriptores: «Phytotherapeutic drugs», «Wounds and injury»,
«Medicinal plant», «Phytotherapeutic drugs», «Wounds and injury», «Medicinal
plant», «Phytotherapeutic drugs», «Heridas y lesiones» y «Plantas medicinales».
Resultados: Se encontraron 325 artículos sobre el tema, de los cuales 39
estaban disponibles en su totalidad. Tras excluir aquellos no relacionados con
el tema, ocho estudios constituyeron la muestra final. Demostraron los impactos
positivos de las plantas medicinales y/o fitoterapéuticos para el tratamiento
de lesiones crónicas en personas de diferentes edades, pero también confirman
la escasez de estudios en esta área. Conclusión: Las plantas medicinales con
propiedades curativas pueden utilizarse de diversas maneras y con distintos
fines según sus compuestos. El análisis de los estudios demuestra su eficacia
en el tratamiento de heridas crónicas.
Palabras clave: Heridas; Cicatrización; Plantas Medicinales.
RESUMO
Objetivo:
Identificar as plantas medicinais e fitoterápicos com efeito cicatrizante para
o tratamento de feridas crônicas. Método: Trata-se de revisão
integrativa realizada no período de janeiro a novembro de 2024, utilizando
artigos publicados dentro dos últimos 10 anos (2013 - 2023), em três idiomas
específicos, português, inglês e espanhol, pelas seguintes bases de
dados/bibliotecas: Biblioteca Virtual em Saúde, Scientific Electronic Library
Online, Portal de Periódicos da Capes, Literatura Latino-Americana e do Caribe
em Ciências da Saúde, e National Library of Medicine, através dos descritores:
“Medicamentos fitoterápicos”, “Feridas e lesões”, “Plantas medicinais”,
“Phytotherapeutic drugs”, “Wounds and injuries”, “Medicinal Plants”,
“Medicamentos fitoterapéuticos”, “Heridas y lesiones”, “Plantas medicinales”. Resultados:
Foram encontrados 325 artigos sobre a temática, sendo 39 disponibilizados na
íntegra. Após a exclusão daqueles que não se relacionavam ao tema, oito estudos
compuseram a amostra final. Exibiu-se os impactos positivos das plantas
medicinais e/ou fitoterápicos para o tratamento de lesões crônicas, em pessoas
de diferentes idades, no entanto, ratificam a escassez de estudos nesta área. Conclusão:
As plantas medicinais com ação cicatrizante podem ser utilizadas de várias
formas e com diversas finalidades de acordo com seus compostos, a análise dos
estudos demonstra sua eficácia no tratamento de feridas crônicas.
Palavras chaves: Feridas; Cicatrização; Plantas
Medicinais.
INTRODUCTION
Human beings can be described as rational beings who, through their
actions, constantly seek to improve their developmental process, which depends
on the integrity of their mental and physical well-being. The skin is the
largest organ of the human body, playing a vital role in defense and in
maintaining homeostasis; however, many factors can impair its proper
functioning. When addressing the treatment of lesions, the professional must
assess the various characteristics presented by the patient and the lesion
itself, including the type of lesion, its etiology and cause, the presence of
odor, type of tissue (granulation, fibrin, or necrosis), exudate (its color and
quantity), and whether the patient reports pain (nociceptive or neuropathic) (1).
Proper assessment of a skin lesion allows the professional to decide
on the best treatment for wound healing or management aimed at the patient’s
comfort. Despite scientific advances regarding wound care, many therapies still
rely on standard substances such as hydrogel, silver sulfadiazine, or those
with antioxidant properties that can be harmful to the formation of healthy
granulation tissue. This may occur due to limited access to more appropriate
products or improper professional conduct, as in the use of hydrogen peroxide,
hypochlorite solution, acetic acid, chlorhexidine, povidone-iodine, and
cetrimide, which, although possessing antibacterial properties, are cytotoxic
to tissue and impair healing (2).
Factors that negatively impact lesion repair slow the healing process
in terms of both anatomical and functional integrity, hindering the biochemical
and cellular processes necessary to maintain skin integrity (3).
Even with the wide range of synthetic substances available for wound
application, areas such as phytotherapy and the use of medicinal plants
represent innovation in dermatological treatment. Although many health
professionals are unaware of the medicinal properties of certain plants, their
use is highly diverse and has been adopted since ancient times in different
cultures (4).
Research highlights the benefits of using medicinal plants and herbal
medicines, commonly associated with the reduction of devitalized tissues,
anti-inflammatory and debriding properties, increased collagen fiber deposition
and cell proliferation, as well as a reduction in healing time and minimal
adverse effects (5).
Medicinal plants have been used for millennia by various cultures to
treat diseases, forming an integral part of traditional medical systems.
However, studies on their use in wound healing remain scarce. Therefore, it is
understood that the population’s knowledge about skin lesion care and the use
of medicinal plants should be integrated with scientific knowledge to expand
research in this field (6).
The use of natural products incorporated into wound care has proven
to be a valuable therapeutic resource. Their inclusion in healthcare
demonstrates versatility, whether used individually or in combination with
other products, showing synergistic potential with conventional therapies.
However, the implementation of such treatments requires professionals to have
greater knowledge of the subject, as merging ancestral knowledge with modern
scientific evidence can be challenging but contributes significantly to global
health (7).
Medicinal plants are those containing substances with healing
properties found in their various parts, leaves, roots, while herbal medicines
are derived from these plants and undergo laboratory processing for their
formulation. Specific substances are extracted for their action, and their
presentation is defined, as creams, tablets, and other forms, expanding the
range of available natural products (8).
Phytotherapy is one of the approaches promoted by the National
Policy on Integrative and Complementary Practices (PNPIC) adopted by Brazil’s
Unified Health System (SUS). Many essential medicines derive from plants with
healing properties and are used in various types of skin lesions such as burns,
pressure injuries, and diabetic foot ulcers, among others. The global
consumption of natural products has increased over the years, and with it, the
adoption of plant-based products with healing action has shown promising
effects for the recovery of skin lesions, whether acute or chronic (8).
The main goal of wound dressing application is complete healing,
achieved through the deposition of various cells in the lesion area to
stimulate granulation tissue formation, the healthy tissue, while promoting
asepsis and protecting the affected area (8).
Therefore, this study aimed to identify medicinal plants and/or herbal
medicines with healing action for the treatment of chronic wounds, addressing
their forms of use and the effectiveness of their implementation.
METHOD
This study consists of an integrative review developed through the
following steps: formulation of the guiding research question, establishment of
inclusion and exclusion criteria, search and evaluation of articles to be
included as the basis of the study, selection of relevant material,
interpretation of results, conclusion, and references.
Initially, the guiding question was formulated as: “Which medicinal plants
and/or herbal medicines are used for the treatment of chronic wounds?” This
question directed the research, with the PICO strategy adopted as follows: “P”
for the use of herbal medicines and/or medicinal plants, “I” for the
intervention by health professionals, and “CO” for existing studies and their
outcomes. This strategy enabled the selection of studies with similar themes,
ensuring exclusivity, relevance, and reliability of the data collected.
The research was conducted in three languages, portuguese, english,
and spanish, across the following databases and libraries: Virtual Health
Library (BVS), Latin American and Caribbean Health Sciences Literature
(LILACS), Scientific Electronic Library Online (SCIELO), CAPES Journal Portal,
and National Library of Medicine (MEDLINE/PubMed). The descriptors used were:
“Medicamentos fitoterápicos”, “Feridas e lesões”, “Plantas medicinais”,
“Phytotherapeutic drugs”, “Wounds and injuries”, “Medicinal Plan”.
Table 1 – Structure of descriptors in databases and libraries used for
data search. João Pessoa, PB, Brazil, 2024.
|
Database
|
Descriptors
|
Results found
|
|
BVS
|
(Phytotherapeutic
drugs) AND (Wounds and injuries) AND (Medicinal Plants).
|
100
|
|
CAPES
|
(Phytotherapeutic drugs)
AND (Wounds and injuries) AND (Medicinal Plants).
|
33
|
|
SCIELO
|
(Phytotherapeutic drugs)
AND (Wounds and injuries) AND (Medicinal Plants).
|
17
|
|
LILACS
|
(Phytotherapeutic drugs)
AND (Wounds and injuries) AND (Medicinal Plants).
|
95
|
|
MEDLINE/PUBMED
|
(Phytotherapeutic drugs)
AND (Wounds and injuries) AND (Medicinal Plants).
|
80
|
The material selection was carried
out independently between January and November 2024. Titles and abstracts were
reviewed, and only articles published in peer-reviewed journals between 2013
and 2023 were included. The software EndNote was used to identify and remove
duplicates and manage references.
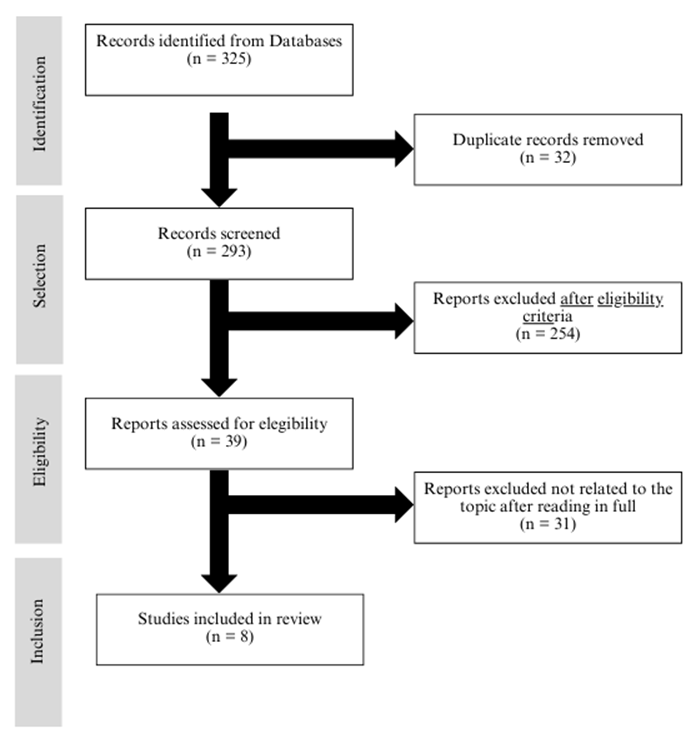
The search yielded 325 articles related to the topic, as shown in
Figure 1. Articles were selected based on title and abstract reading, applying
inclusion and exclusion criteria, and removing duplicates. Studies that used
herbal medicines and/or medicinal plants in skin lesions and were indexed in
databases between 2013 and 2023 were included, while theses, dissertations,
monographs, and papers not addressing the guiding question were excluded.
Figure
1
– Flowchart of study identification, selection, and inclusion, using the
Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA).
João Pessoa, Paraíba, 2024.
RESULTS
The search yielded a total of eight
articles selected for its composition, as described in table 2, which consists
of the items: work title, year/country of origin, database, type of study,
objective, medicinal plant/herbal medicine, form of use, type of lesion, and
results. The description of the bibliographic material that constitutes the
present study exhibits scientific productions from different databases and
indexed libraries. From the material selected for the research, relevant
information was extracted regarding eighteen types of different medicinal
plants and/or herbal medicines, as specified in table 2, highlighting the
variety of their use and the types of chronic lesions addressed.
DISCUSSION
This research addresses the treatment
of chronic wounds, which significantly impact the patient's quality of life.
Because they are complex wounds, they may require multifocal care, meaning that
the lesions must be evaluated in all their aspects. This is one of the benefits
of medicinal plants and phytotherapeutic products, as their properties do not
involve only one aspect of the pathology (1).
Chronic wounds are those that are
difficult to heal, and their healing process is more complex compared to that
of acute lesions. Comprehensively, it involves evaluating the patient's
nutritional aspects, infection control, adequate asepsis, wound bed preparation,
infection prevention, debridement, and preservation of the wound bed,
stimulating the emergence of healthy granulation tissue and its
epithelialization (2).
In the health field, there is much
discussion regarding the benefits and harms of using medicinal plants and/or
herbal remedies. Given that the population regularly uses these natural
products, it is up to the professional to have knowledge of the subject in
order to provide guidance, as well as to contribute to effective research for
clinical use.
Throughout
the research, the use of various medicinal plants and herbal medicines was
observed, both in isolation and as a complementary therapy in the healing
process. The composition of these natural products is usually complex, due to
the variety of active ingredients that confer their medicinal properties.
An example is
Calendula officinalis oil, a plant originating in the Mediterranean and
popularly known as Marigold (Calêndula in Portuguese), which is rich in
Essential Fatty Acids (EFAs). Due to its anti-inflammatory, therapeutic, and
healing effects, the National Health Surveillance Agency (ANVISA) recommends
its topical use in the treatment of chronic lesions (2).
The
consumption of natural products has gained prominence due to its association
with a healthy lifestyle. However, the use of medicinal plants is an ancient
practice, employed not only in the treatment of wounds but also for various
health conditions, such as neoplasms, conjunctivitis, hyperglycemia, and
dyslipidemia.
Among these
plants, Aloe vera (popularly known as Aloe) stands out in the treatment
of skin lesions. Widely known in Brazil, it presents anti-inflammatory,
antioxidant, healing, bactericidal, and laxative effects. This is thanks to its
rich composition of vitamins, enzymes, minerals, sugars, salicylic acid, and
amino acids. Scientific evidence demonstrates that its use can reduce pain in
chronic lesions and accelerate the healing process (5).
Medicinal
plants and/or herbal medicines used to restore tissue integrity may share some
common effects, such as anti-inflammatory, antimicrobial, wound-healing, and
analgesic actions, as seen in the previous examples with Aloe vera and Calendula
officinalis. However, their form of presentation varies, based on the
extraction method used and the type of plant. In a case study involving an
ointment made from 0.2% Hyaluronic Acid extracted from fruits, 10% glycolic
Papain extract, Aloe vera extract, Andiroba extract, Rosemary oil, Tea
Tree oil (Melaleuca), and Copaiba oil, it was demonstrated that, despite
its complex composition, it was capable of epithelializing a traumatic,
chronic, complex, and difficult-to-heal wound (4).
Given the
function of the healing process, the application of natural products and
improvements in their use are described in studies that indicate fast-acting
products, some with an efficacy of 90% to 100% epithelialization, with
monitoring mostly performed by nurses. Control is achieved through the use of
patient records, clinical progression, and nursing progress notes, which
monitor the healing process with the aim of conducting appropriate treatment,
planning, and interventions based on the specific needs of the patient and
their lesion (6).
The research
analyzed in this 10-year period (2013-2023) highlights several plant species
with extracts of proven efficacy in therapeutic applications, including Aloe
vera (L.) Burm.f. (Aloe), Calendula officinalis L. (Pot Marigold),
the oil extracted from the seeds of Rosa canina L. (Rosehip), and Carica
papaya L. (Papaya). In a study with patients in the postoperative period of
open hemorrhoidectomy, the use of an Aloe vera-based cream resulted in
less pain, accelerated healing, and reduced analgesic consumption. Furthermore,
its efficacy in the treatment of second-degree burns, in a group of 30
individuals, was proven in a comparison with 1% silver sulfadiazine (standard
treatment); a cream containing 0.5% Aloe vera promoted faster
re-epithelialization and reduced lesion size compared to the control group,
reinforcing its potential as an effective therapeutic alternative (5).
The
literature reviews, clinical trials, and other research analyzed in this study
show the good acceptance of medicinal plants and/or herbal medicines used not
only for superficial lesions, such as peristomal dermatitis, but also for
varied chronic wounds, such as diabetic wounds, pressure ulcers, and even
lesions with bone exposure. As we can see, the observed lesions are quite
varied, and one of the innovations found was the use of Neem and Hypericum oil
(Holoil), in cream form, to treat skin ulcers related to calcinosis in systemic
sclerosis. Patients who applied the cream daily showed reduced pain and
prevalence of infections, as well as the crushing and complete resolution of
calcium deposits, facilitating their excision during wound treatment sessions.
This efficacy demonstrated the complete healing of 15 out of 33 patients (6).
Despite their
proven efficacy, a major barrier to the implementation of medicinal plants
and/or herbal medicines for the treatment of skin lesions, such as wound
healing, arises when health professionals do not seek contact or improvement of
phytotherapy knowledge in this field, which results in reduced innovations,
even though this treatment option has shown, according to research, relevant
results in the recovery of injured tissue, and also presented lower cost and
few adverse effects (8).
Similarly,
another reported limitation involves some research where, before using
medicinal plants and/or herbal medicines, health professionals use standard
therapies, that is, products commonly known for use in the area, already
recommended substances (depending on the lesion), such as Activated Charcoal,
Hydrogel, Silver Sulfadiazine—making the effectiveness of the herbal medicine
inconclusive, which is detrimental to data collection for future research in
the area (8).
In contrast
to the barriers identified through the study, there are still innovative
developments in the health field related to the use of medicinal plants and/or
herbal medicines as viable treatment options for chronic lesions. A study
involving the application of a spray composed of Neem oil and Hypericum
perforatum L. in patients with postoperative scalp wounds with exposed
bone, developed in Switzerland, showed results with positive impacts on lesion
healing. The herbal medicine, with antimicrobial effect, prevented the
secondary dressing from adhering to the wound bed, preserving wound moisture.
In a sample containing 15 patients, 7 had the exposed area 100% covered, due to
the high potential for granulation tissue emergence at the site, with no reports
of intense pain or adverse effects recorded (10).
Such research
highlights how medicinal plants with wound-healing action can be used in
various ways and for different purposes according to their compounds,
potentially leading to herbal medicines that potentiate their effects. Plants
rich in tannins favor epithelialization and cell proliferation, which justifies
the high potential for promoting the emergence of granulation tissue, while
species rich in quinones, naphthoquinones, and flavonoids have antibiotic and
anti-inflammatory action. Furthermore, knowing the proper handling and use
shows that different parts of the plant can be used, such as leaves, roots, or
stems, and these have varied preparation forms, being found as decoctions,
tinctures, and even ointments (16).
The discussed
research reports different types of treatment for skin lesion care, and that
the regeneration process is intensified by focusing on increasing the
deposition of cells that restore the tissue. The wound healing process has
three distinct phases: the inflammatory process, where damaged cells and
pathogens undergo phagocytosis; the cell proliferation process for new tissue
formation and angiogenesis, aiming for the emergence of granulation tissue; and
finally, the tissue remodeling stage, through collagen deposition (16).
The healing
process of a chronic lesion differs from an acute lesion due to its complexity,
especially in the inflammatory phase of the lesion, which is more prolonged due
to the high and unbalanced deposition of monocytes and pro-inflammatory M1
macrophages, which directly impacts epidermal re-epithelialization. That said,
the professional must take into account the high complexity of the lesion and
all the barriers that slow down healing when performing the dressing, ensuring
patient safety. Despite this, many conventional techniques and dressings do not
meet these demands, leading researchers to focus on natural products (11).
The plant
genera used topically found in the research, such as Aloe, Anacardium,
Rosa, Calendula, among many others cited, have wound-healing,
bactericidal, and anti-inflammatory action, which is due to their composition
rich in tannins, flavonoids, and phenolic acids. Their diverse mechanisms of
action, stemming from these varied compounds, show that they can be as
efficient as pharmaceutical products like antibiotics, even without their
therapeutic selectivity (11).
The
understanding of the positive impact that the use of phytotherapy can provide
for the care of skin lesions raises the question of why its products are so
little utilized. Studies on medicinal plants and/or herbal products for topical
use on skin wounds are still scarce, the vast majority being limited to animal
use, despite studies showing scientific evidence for use in humans, making this
an area that needs to be explored to improve the treatments used and the
quality of healthcare for patients (11,16).
Possessing
the appropriate knowledge related to physiology, the mechanism of wound
healing, exudate, signs of infection, and biofilms is essential to treat a
lesion adequately. Difficult-to-heal wounds often result from the increased
incidence of preventable problems, such as Diabetes Mellitus and rising
obesity, becoming a public health issue that affects countless people and a
challenge for health professionals (11,12).
Taking common
comorbidities as an example, Diabetes Mellitus, a disease associated
with insulin deficit resulting in high blood sugar levels (hyperglycemia), if
not properly treated, has the development of Diabetic Foot Ulcers (DFU) as one
of its main consequences. Understanding this daily problem is fundamental for
the professional who provides care for skin lesion treatment, with diabetic
foot ulcers being the most explored type of lesion in ethnobotanical research.
Such studies are due to common actions such as the antioxidant effect
(neutralizing free radicals and reducing oxidative stress); improvement of
angiogenesis; acceleration of healing (stimulating greater collagen
deposition); and antimicrobial effect (preventing colonization), these actions
being respective of plants like Calendula officinalis, Teucrium
polium, Actinidia deliciosa, and Aloe Vera (12).
Another
common type of lesion identified in the research was pressure ulcers or
pressure injuries (PU), which result from friction or pressure in a localized
area, associated with medical devices or the need for repositioning, leading to
compromised dermal integrity. A study using Neem and Hypericum oil, which was
used to produce an herbal medicine in the form of an ointment for three
bedridden patients in an ICU (Intensive Care Unit), was conducted over a period
of 42 consecutive days. The ointment was applied once a day. Due to
histological monitoring, it was possible to observe that the lesioned patients
showed total healing of the lesion in an average time greater than or equal to
42 days. By exhibiting its potential, the herbal ointment proves to be an
effective alternative for the treatment of these lesions. However, the research
sample was relatively small, which again raises the issue of the need for more
research in the area, confirming its viability (17).
The research
analyzed in this work highlighted the positive impact of using medicinal plants
and herbal medicines in the topical treatment of wounds, demonstrating the
evolution of their application throughout history. Originally, their main
purpose was to stop hemorrhages and promote healing, being mostly administered
orally for systemic absorption. In discussing the range of benefits in the
production of herbal medicines and the use of traditional plants, the research
also portrays their relevance from a socioeconomic perspective, as the cost of
implementing more natural products to treat chronic lesions represents a more
viable alternative, justifying the rise in their use. Currently, these
substances present various pharmaceutical forms, including innovative
formulations such as oils, powders, and sprays, which expand their therapeutic
efficacy and convenience (13,18).
A study
involving Rosa aff rubiginosa or Rosa canina L, popularly known
as Rosehip, highlighted the therapeutic potential of the agent, which has
anti-inflammatory, immunomodulatory, cardioprotective, antimicrobial, and
antioxidant actions. In Brazil, the plant is mainly used in the form of oil,
extracted from the seed for the production of herbal medicines, with a
composition rich in polyphenols, carotenoids, ascorbic acid (Vitamin C),
unsaturated fatty acids, and transretinoic acid, contributing to the maintenance
of skin integrity and its healing. Studies affirm that skin lesions treated
with Rosa canina L. oil showed greater deposition of collagen and
fibroblasts, reduced edema, and the rapid emergence of granulation tissue,
corroborating the reduction of the lesion area in a shorter time (19).
Innovations
in the area have allowed the treatment of various types of lesions, such as
peristomal dermatitis, a common chronic lesion in patients with intestinal
ostomies, characterized by inflammation, pain, and compromised skin integrity
around the stoma. In this context, a study investigated the therapeutic use of Musa
sapientum (green banana), through the application of an herbal powder
containing 10% of the fruit peel, formulated with the addition of gelatin and
carboxymethylcellulose. The product was applied directly to the lesion, once a
day, in adult ostomy patients. The results showed that the group that used the
powder had a significantly shorter healing time compared to the control group (p=0.022),
in addition to reporting pain relief, a sensation of comfort, and skin
protection with effective moisture absorption. These findings highlight the
efficacy of the green banana-based herbal medicine as a viable and low-cost
alternative for the treatment of peristomal dermatitis, demonstrating its
wound-healing and anti-inflammatory potential (14).
The
improvement of the functionality of the various compounds present in medicinal
plants allows the development of herbal medicines, and although research
affirms the scarcity of studies related to this theme, there are some
consolidated herbal medicines on the market, among them, those whose
formulation includes papain, a proteolytic enzyme used primarily for the
treatment of lesions with the presence of devitalized tissue. In this regard, a
study with a patient containing a DFU, with an extent of 24 cm², granulation
tissue in the wound bed, and macerated edges, using an herbal ointment applied
once a day, over a period of 1 month and 3 days, composed of 10% papain and
hyaluronic acid, its use provided chemical debridement, helped combat
colonization due to antimicrobial properties, promoting the emergence of
healthy tissue and stimulating healing (15).
The
construction of the research highlighted that other studies addressing this
theme reveal that medicinal plants and/or herbal medicines used for skin
lesions demonstrate efficiency in their healing potential, acting in the
recovery of the individual's physiological and anatomical functions, in
addition to presenting benefits related to ease of production and low cost (20).
Addressing
the topic of medicinal plant use, broadly, from the perspective of improving
human quality of life, brings up how the knowledge of the benefits of
phytotherapy practices is intertwined with social knowledge. Some research
addressing the theme of medicinal plant and herbal medicine use surveys
different types of plants used in different regions by the population.
Ethnobotanical resources hold great relevance in the treatment of various
diseases and skin lesions, meeting the basic needs of a population as an
alternative form of treatment to conventional methods (21).
From this
analysis, such information and its uses must be perpetuated and are enhanced
thanks to technical-scientific advances. The professionals responsible for
providing care for skin lesions, and who are directly related to the function
of performing dressings, are of utmost importance for the lesion to achieve
good healing and for the patient to be cared for holistically (22).
CONCLUSION
The use of
medicinal plants and/or phytotherapeutic products in the treatment of skin
lesions demonstrates a beneficial potential in the tissue repair mechanisms of
individuals. The research discussed not only recovers the age-old use of these
methods, but also presents studies that demonstrate innovation in the area,
their use in chronic lesions, and how they facilitate the process by
accelerating the appearance of granulation tissue, due to their active
ingredients that contribute to the appearance of healthy tissue. This work
defines the importance of adopting phytotherapy for use in skin lesions, as a
way to promote its use in current practices. The understanding of this
complementary treatment by health professionals can result in several benefits,
thus contributing to scientific advancement in the development of advanced
methods for treating skin lesions in humans.
REFERENCES
1. Buzzi M, de
Freitas F, Winter R, Siviero A, Nampo FK. A prospective, descriptive study to
assess the clinical benefits of using Calendula officinalis
hydroglycolic extract for the topical treatment of diabetic foot ulcers. Ostomy
Wound Manage. 2016 Mar;62(3):8–24.
2. Carvalho AFM,
Feitosa MCP, Coelho NPMF, Rebêlo VCN, Castro JG, Sousa PRG, et al. Low-level
laser therapy and Calendula officinalis in repairing diabetic foot
ulcers. Rev Esc Enferm USP. 2016;50(4):628–634.
3. Chini LT, Muniz
RM, Neves ET, Silva ÍR, Corrêa AR. O uso do Aloe sp (Aloe vera) em
feridas agudas e crônicas: revisão integrativa. Aquichan. 2017.
4. Cruz CLS, Silva
MA, Nascimento RS, Almeida JDS, Silva Júnior JF. Tratamento de feridas com
utilização de fitoterápico em paciente vítima de atropelamento: relato de caso.
Rev Enferm Atual In Derme. 2022;96(40): [s.p.]
5. Freitas VS,
Rodrigues RAF, Gaspi FOG. Propriedades farmacológicas da Aloe vera
(L.) Burm. f. Rev Bras Plant Med. 2014;16(2):299–307.
6. Giuggioli D,
Colaci M, Murdaca G, Lumetti F, Ferri C. Use of Neem oil and Hypericum
perforatum for treatment of calcinosis-related skin ulcers in systemic
sclerosis. J Int Med Res. 2020 Jan;48(4):0300060519882176.
7. Juvino ER,
Mariz SR, Félix LG. Os produtos naturais na cicatrização de feridas cutâneas em
ambiente hospitalar: práticas e saberes dos profissionais de enfermagem. Rev
Enferm Atual In Derme. 2021;95(34): e-021049.
8. Kloter E, Nardi
GM, Alves RMP, Pereira SMS, Silva FFC. Phytotherapy in paediatric skin
disorders - A systematic literature review. Complement Ther Med. 2023
Apr;74:102933.
9. Buzzi M,
Freitas F, Winter MB. Cicatrização de úlceras por pressão com extrato
Plenusdermax® de Calendula officinalis L. Rev Bras Enferm.
2016;69(2):250–257.
10. Läuchli S,
Eich D, Böttcher-Haberzeth S, Meuli M, Turina M, Stähli A, et al. A
plant-derived wound therapeutic for cost-effective treatment of post-surgical
scalp wounds with exposed bone. Forsch Komplementmed. 2014;21(2):88-93.
11. Moses RL,
Prescott TAK, Mas-Claret E, Steadman R, Moseley R, Sloan AJ. Evidence for
natural products as alternative wound-healing therapies. Biomolecules.
2023;13(3):444.
12. Narzary I,
Swarnakar A, Kalita M, Middha SK, Usha T, Babu D, Mochahary B, Brahma S,
Basumatary J, Goyal AK. Acknowledging the use of botanicals to treat diabetic
foot ulcer during the 21st century: A systematic review. World J Clin Cases.
2023;11(17):4035.
13. Rayate AS,
Pawar S, Pawar S, Singh K. Current scenario of traditional medicines in
management of diabetic foot ulcers: A review. World J Diabetes. 2023;14(1):1.
14. Silva AC,
Silva MM, Lima FJ, Souza LD, Costa MM. Peristomal dermatitis: treatment with
green banana peel (Musa sapientum) powder. Coloproctol (Rio J).
2021;41(2):145-151.
15. Teixeira AR,
Silva LMB, Costa RM, Almeida FS. A utilização de fitoterápicos no tratamento de
feridas diabéticas: relato de caso. Rev Enferm Atual In Derme. 2022;96(40).
16. Moreski DAB,
Prado FM, Cardoso TN, Souza FC, de Carvalho DC. Ação cicatrizante de plantas
medicinais: um estudo de revisão. Arq Cienc Saúde UNIPAR. 2018;22(1).
17. Özdemir S,
Bostanabad SY, Parmaksız A, Canatan HC. Combination of St. John's Wort Oil and
Neem Oil in Pharmaceuticals: An Effective Treatment Option for Pressure Ulcers
in Intensive Care Units. Medicina (Kaunas). 2023;59(3):467.
18. Piriz MA,
Gutiérrez SM, Lima JMG, Souza LP. Uso popular de plantas medicinais na
cicatrização de feridas: implicações para a enfermagem. Rev Enferm UERJ.
2015;23(5):674-679.
19. Santos JS,
Barreto LCLS, Kamada I. Rosa mosqueta como potencial agente cicatrizante. Rev
Cuba Enferm. 2018;e1235-e1235.
20. Vargas NRC,
Petry AF, Marin MJS, Modolo LV. Plantas medicinais utilizadas na cicatrização
de feridas por agricultores da região sul do Rio Grande do Sul. Rev Enferm
UFSM. 2014.
21. Vieira LS,
Sousa RS, Lemos JR. Plantas medicinais conhecidas por especialistas locais de
uma comunidade rural maranhense. Rev Bras Plantas Med. 2015;17(4):1061-1068.
22. Zago LR,
Santos DCS, Oliveira MF, Santos ALQ, da Silva RHC. The use of babosa (Aloe
vera) in treating burns: a literature review. Braz J Biol. 2021;83:e249209.
Funding and
Acknowledgments
The authors
declare that this research received no funding.
Conflict of
Interest Statement:
The authors
declare no conflicts of interest.
Data Availability
Statement:
No databases were
generated in this study. The information presented is described in the body of
the article.
Authors'
Contributions:
All authors
contributed to the study planning, data analysis and interpretation, as well as
the writing for the final published version.
Scientific Editor:
Ítalo Arão Pereira Ribeiro. Orcid:
https://orcid.org/0000-0003-0778-1447
Rev Enferm Atual
In Derme 2026;100(1): e026018

